Welcome to NUCMEDCOR
NUCMEDCOR (NMC), an ISOFLEX USA (IUSA) company, is a distributor of high-quality nuclear medicine products supporting the nuclear medicine industry. Our product offering includes biochemical compounds used in the synthesis of radiopharmaceuticals, as well as vials, cassettes, reagent kits and other consumables for molecular imaging. Additionally, we have an extensive catalog of radiation shielding products.
In order to keep pace with the demands of the molecular imaging community, NMC will continue to add products to support nuclear medicine. We welcome your inquiries for custom synthesis applications and long-term supply agreements.
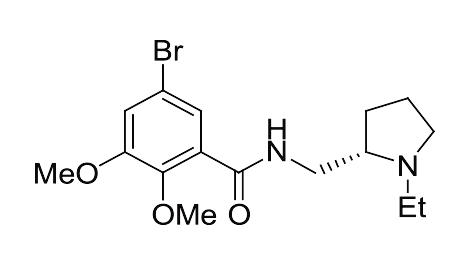
We are pleased to offer a broad selection of PET and SPECT precursors, reference standards and reagent kits. Our products have been developed for the production of [18F]FDG, FLT, FMISO, F-Choline and F-DOPA with the following synthesis modules:
All of our consumables and accessories are produced with full cGMP compliance. We offer custom clean-room packaging for all quantities. Visit our product pages for details:
Our Oxygen-18 (O-18/18O) is manufactured according to cGMP, ISO-9001:2008 and ISO-14001:2004 standards. We offer the following forms of O-18 with a variety of packaging options, as well as one-time and long-term delivery contracts:
Oxygen-18 Enriched Water (10 Atom %)
Doubly Labeled Water (10 Atom %)
Check out our O-18 recycling program as well, which can help reduce your purchase price significantly.
Need immediate assistance? Give us a call: (415) 440-4433